Cardiology: Invasive
Invasive Cardiology Services in Arizona
Diagnostic Cardiovascular Catheterization
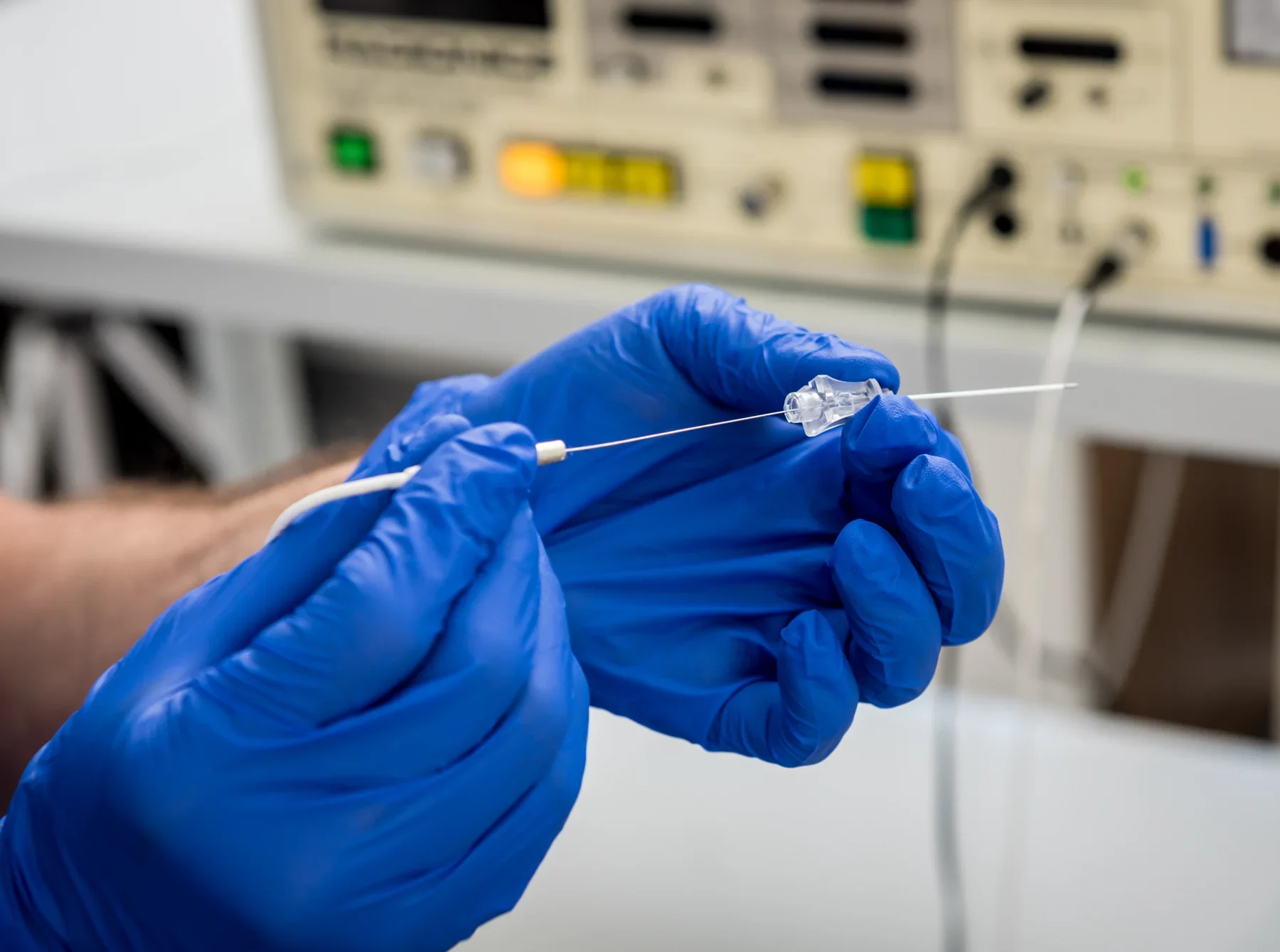
Cardiac catheterization, also known as a ‘cardiac cath,’ is frequently used for diagnosis and treatment of a wide variety of heart conditions. This procedure involves a long thin tube (the catheter) being inserted into an artery in the patient’s arm, groin, or veins of groin or neck, and then guided through the circulatory pathway to the heart.
Cardiac catheterizations may be done to assess coronary arteries for blockages and/or to assess the status of heart valves. Blood pressures in the various chambers of the heart and lungs can be measured to determine the function of the heart. Depending on the findings, a coronary intervention may be undertaken to place a stent into the diseased artery.
Right Heart Catheterization
Cardiac catheterization, also known as a ‘cardiac cath,’ is frequently used for diagnosis and treatment of a wide variety of heart conditions. This procedure involves a long thin tube (the catheter) being inserted into an artery in the patient’s arm or groin, and then guided through the circulatory pathway to the heart. In a right-heart catheterization, the doctor guides a special catheter (a small, hollow tube) called a pulmonary artery (PA) catheter to the right side of the heart. He or she then passes the tube into the pulmonary artery. This is the main artery that carries blood to the lungs. The doctor observes blood flow through the heart and measures the pressures inside the heart and lungs.
Your doctor may do a right-heart catheterization to see how well or poorly your heart is pumping, and to measure the pressures in your heart and lungs. This test is also known as pulmonary artery catheterization.
As the catheter advances toward your pulmonary artery, your doctor measures pressures along the way, inside the chambers on the right side of your heart. This includes the right atrium and right ventricle. Your doctor can also take indirect measurements of pressures on the left side of your heart. Your cardiac output—the amount of blood your heart pumps per minute—is also determined during a right-heart cath.
Right heart catheterization is used to diagnose or manage:
- Heart failure. A condition in which your heart muscle has become so weak, it can’t pump blood efficiently. This causes fluid buildup (congestion) in your blood vessels and lungs. Fluid may also buildup in your feet, ankles, and other parts of your body.
- Shock. This causes reduced flow of blood and oxygen to the tissues of your body. Sudden onset of heart failure, severe bacterial infection of your blood stream (sepsis), or severe blood loss (hemorrhagic) can cause shock.
- Congenital heart disease. These are birth defects that develop in the heart. An example is ventricular septal defect. This is a hole in the wall between the lower chambers of your heart.
- Heart valve disease. Malfunction in one or more of your heart valves may interfere with normal blood flow within your heart.
- Cardiomyopathy. This is an enlargement of your heart due to thickening or weakening of your heart muscle. It can eventually lead to heart failure.
- Pulmonary hypertension. Increased pressures in the blood vessels in your lungs. This can lead to trouble breathing and right-sided heart failure.
Coronary Angiography
Coronary Stenting
Transradial Catheterization
Rotational Atherectomy
Transesophageal Echocardiography
TEE can be used to determine:
- The size of your heart and how thick its walls are.
- How well your heart is pumping.
- If there is abnormal tissue around your heart valves that could indicate bacterial, viral or fungal infections, or cancer.
- If blood is leaking backward through your heart valves (regurgitation) or if your valves are narrowed or blocked (stenosis).
- If blood clots are in the chambers of your heart, in particular the upper chamber, for example after a stroke.
Electrical Cardioversion
Abnormal heart rhythms are called arrhythmias and they may prevent blood from circulating properly to your heart and brain. If your heart has an irregular (uneven) beat or is beating too fast, cardioversion is a way to restore a regular rhythm. Electrical cardioversions restore regular rhythms by sending an electrical shock to the heart.

PFO Closure
All human fetuses have a hole in the wall between the left and right atria called the foramen ovale. This hole allows blood to bypass the lungs while in utero. After birth, the foramen ovale closes, and within a few months it has sealed completely in most humans. When it remains open, it is called a patent (open) foramen ovale (PFO).
For the vast majority of the millions of people with a PFO, it is not a problem and does not require any treatment, even though blood is leaking from the right atrium to the left. Problems can arise when that blood contains a blood clot. Using standard cardiac catherization techniques, a catheter can be used to guide the placement of a patent foramen ovale (PFO) closure device that will close the hole (prevent the flap from opening) in the heart wall. The device becomes a permanent implant.
Valvuloplasty
A valvuloplasty, also known as balloon valvuloplasty or balloon valvotomy, is a procedure to repair a heart valve that has a narrowed opening.
In this valve condition, the valve flaps (leaflets) may become thick or stiff, and they may fuse together (stenosis). This causes the valve opening to be narrowed and results in reduced blood flow through the valve.
If you have severe valve stenosis we may recommend a valvuloplasty to repair a mitral valve, aortic valve, or pulmonary valves. This procedure involves inserting a long, thin catheter with a balloon on the tip into an artery in your arm or groin. The catheter is guided to the valve using X-ray imaging. The ballon is then inflated, which expands the opening of the valve and separates the leaflets. The balloon is then deflated, and the catheter and balloon are removed.
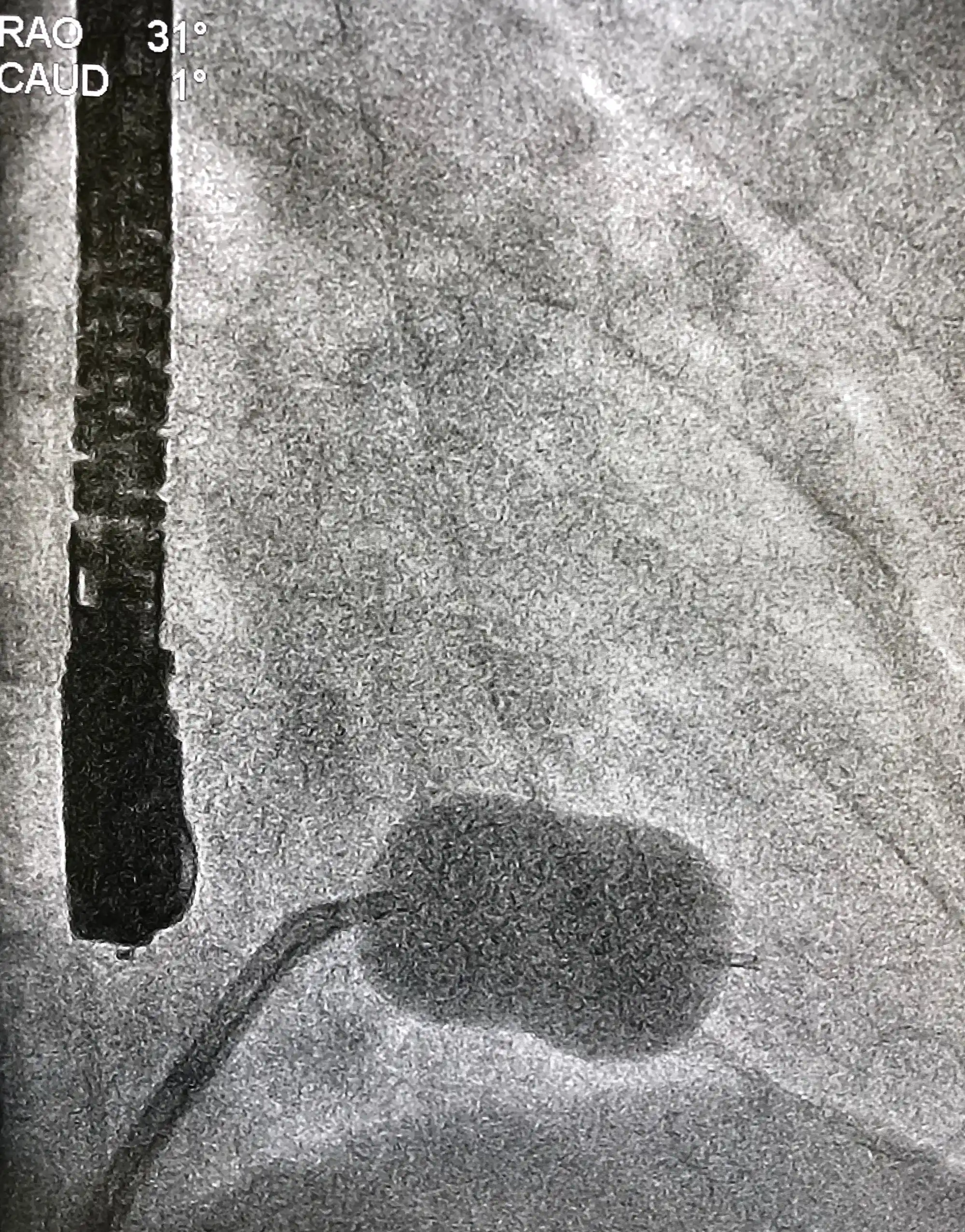
Chronic Total Occlusion (CTO)
Chronic Total Occlusion is a nearly complete blockage of one or more arteries, caused by a build up of plaque. The blockage is typically present for more than 3 months and the blockage compromises blood flow to the heart. Approximately 30% of all patients with coronary artery disease will experience chronic total occlusion.
Symptoms are typically observed during activity and may include:
Patients are at a greater risk for developing Chronic Total Occlusion if they are smokers or are obese, and if they have high cholesterol, diabetes, high blood pressure and/or coronary artery disease, or if they have a history of heart attack.
Chronic total occlusion is typically diagnosed with coronary angiography and possible treatments include medication, coronary artery bypass graft (CABG), and the more minimally invasive percutaneous coronary intervention or PCI.
- Chest discomfort (pain, pressure or tightness)
- Shortness of breath
- Dizziness
- Fatigue
- Nausea
- Pain in the arm or upper body
- Rapid or irregular heartbeat
